As Indiana braces for surge, state officials mum on number of ICU beds and ventilators for COVID-19 patients, as partial picture for beds starts to emerge in Bloomington area

A numerical tally of specific hospital resources that are available to treat Indiana’s COVID-19 patients is not information that state health officials are eager to provide.
When asked at the daily press briefing on Thursday, for the number of ventilators and intensive care unit (ICU) beds that are available, Kristina Box, the state’s health commissioner, declined to say. She cited the confidentiality that hospitals expect when they submit their information to the state.
The question was again rebuffed at Friday’s briefing. On both days, there was some hint that a breakdown of aggregated region-by-region numbers could made available, so that the resources available at a specific hospital would not be revealed.
Shelli Yoder, who’s vying with John Zody and Trent Feuerbach for the Democratic Party’s nomination in the race for the District 40 state senate seat, issued a press release on Saturday morning calling on Indiana’s governor, Eric Holcomb, to release the numbers. The press release says Yoder has sent a letter to the governor that among other things states:
The people of Monroe County are demanding to know:
(1) How many critical care beds do we have available?
(2) How many ventilators do we have available?
(3) What types of healthcare equipment to keep our medical professionals and
frontline responders safe do we have available?
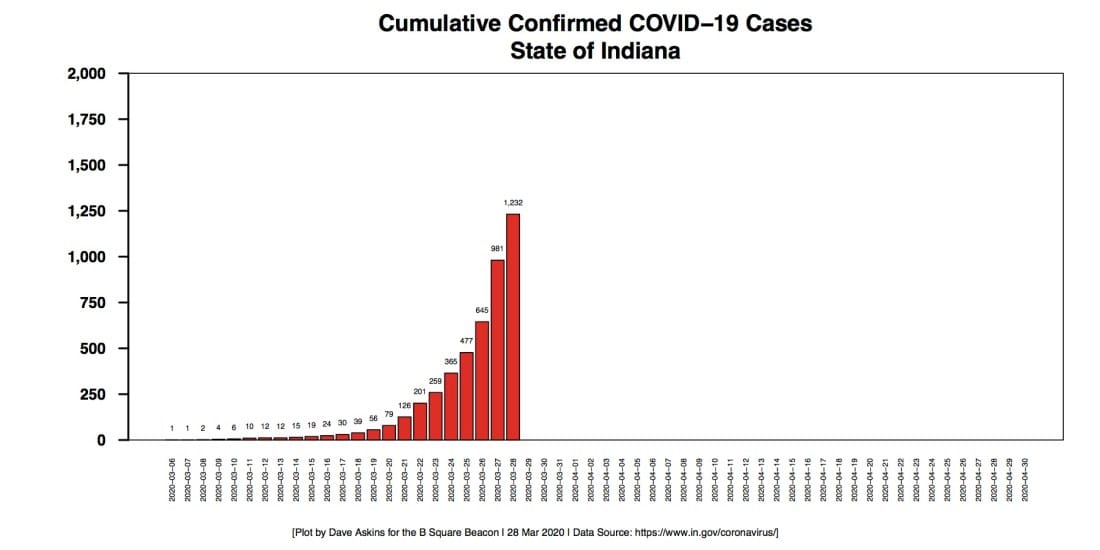
The push for more information comes as the number of cases continues to climb. The number of confirmed COVID-19 cases in Indiana has about doubled (x 1.9) in two days, from 645 on March 26 to 1,232 on Saturday, March 28. The number of tests has increased by a similar factor, for the same period, from 4,651 to 8,407.
In the same two-day period, the number of Hoosiers killed by COVID-19 almost doubled, from 17 to 31.
On Friday, about the idea of providing region-by-region numbers for ventilators and ICU beds, Indiana governor Eric Holcomb said, “We can look toward that. I want to make sure we’re not violating any law or agreement with the hospitals.”
Why are state officials refusing to release the information?
On Friday, Box sketched a scenario where she gave a specific number for capacity, and the number of patients rose to 99 percent of capacity. “Everyone starts to get extremely excited, and upset and worried about that,” she said.
The number of ICU beds isn’t fixed, Box said, because as capacity is reached, other areas can be opened up. Holcomb alluded to “alternative measures, in the event that the number of currently available beds isn’t enough.
Holcomb said, “Right now we know we that have the inventory to handle where we are today…as we get to those numbers spiking or closer to that peak, we’ll keep the public informed of alternative measures we may have to take.” He added, “Hopefully we don’t have to take those… that’s why it’s important that we practice social distancing.”
At Friday’s local press briefing in Bloomington, some of the alternative measures IU Health is taking at its Bloomington hospital were described by Brian Shockney, president of IU Health’s South Central Region.
The picture Shockey gave on Friday included more detail than the one he sketched at Monday’s briefing.
On Friday, Shockney confirmed that the hospital has 272 beds and that, in principle, all the rooms where those beds are located can be converted to a negative pressure environment. That means the space is ventilated in a way that lets air flow into the room but not escape from the room, which helps avoid room-to-room contamination.
“We continue every day to bring more rooms up to negative pressure,” Shockney said.
Shockey also said the strategy for adding beds is to focus first onsite, as opposed to looking at offsite locations. Without disclosing where they are, he confirmed that offsite locations are also a part of the hospital’s “surge plan.”
Among the specific tactics the Bloomington facility is using to add capacity onsite, Shockney described converting the sleep study area to patient care.
Shockey also described an agreement the hospital has made with Ivy Tech to use the nursing education facility for patients discharged from the hospital who can’t return home because someone at their home has COVID-19.
Over the years, some areas at the hospital have been turned into surgical check-in areas. Now that only emergency surgery is being done, Shockney said, those check-in areas can be used for patient care.
With the additional beds that the hospital has added onsite, Shockney pegged the total number at over 300.
He also pointed to IU Health hospitals in Bedford and Paoli as offering available capacity for the region. According to American Hospital Directory, Inc., the Bedford facility has 25 beds. Paoli adds another 24 beds.
Concern about hospital capacity is driven not by current numbers of COVID-19 patients, but by projections for peak numbers. Over the last week, the word “surge” has been used with increasing frequency by officials on both the state and local levels .
At Friday’s press briefing, Box said the models her office is using put the peak of the pandemic in Indiana coming in mid- to late-April. She declined to give a best-guess estimate of what kind of numbers that would mean.
The timeframe Box gave is consistent with a model released on Friday by the Institute for Health Metrics and Evaluation (IHME). The institute is a health research center at the University of Washington.
For Indiana, the IHME model forecasts the peak use of hospital resources to come around April 14.
At the peak of the COVID-19 pandemic, the model predicts that a total of 10,458 beds will be needed statewide, compared to the 8,485 available beds assumed by the study.
The model also predicts that 1,582 ICU beds will be needed, more than twice the 706 ICU beds that are available, according to the study. Finally, the model forecasts that 854 ventilators will be needed.
The IHME study does not include numbers of available ventilators.
The total number of deaths caused by COVID-19 in Indiana is forecast by the IHME study to be 2,440. The peak number of COVID-19 deaths for any day is forecast to be be 110, coming on April 14.




Comments ()